Structure of Eye
The eye is a complex organ that converts light rays to images by means of nerve impulses that feed into the brain. To understand the eye and the eye disorders, we can have the eye in two parts – the anterior and the posterior.
- The Anterior of the eye consisting of the Sclera (the white of the eye) and the Cornea.
- The Posterior of the eye consisting of the Retina (the back of the eye), the Optic Nerve (sending impulses to the brain translating the image), the Iris (the fluid containing colored part of the eye) and the Macula (the highly sensitive area of the retina responsible for focusing).
How Eye Works?
- When you look at an object, light rays are reflected from the object to the cornea.
- Light rays pass through the cornea, which does most of the focusing
- The pupil in the Iris opens to let in more light when its dark, and closes to let in less when its bright
- The lens fine tunes the focusing Here at the retina, the light rays are converted to electrical impulses that are then transmitted through the optic nerve, to the brain, where the image is translated and perceived in an upright position.
Cataract
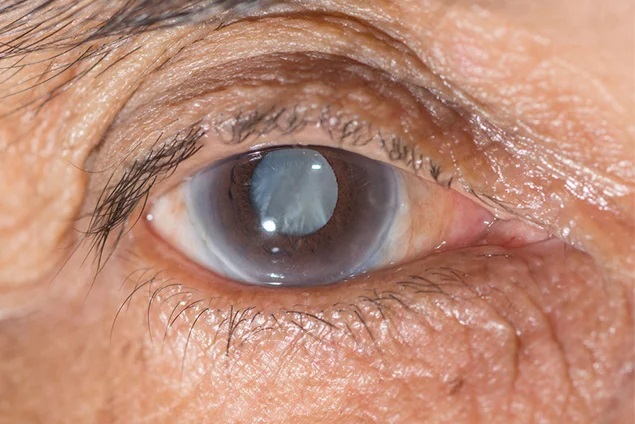
Cataract formation is a natural part of aging. Cataract surgery, a common and successful procedure with a 98% success rate, typically restores vision with microsurgery. Patients experience minimal discomfort and can usually return home a few hours after surgery. Here is what to expect before, during, and after the procedure.
The Surgery
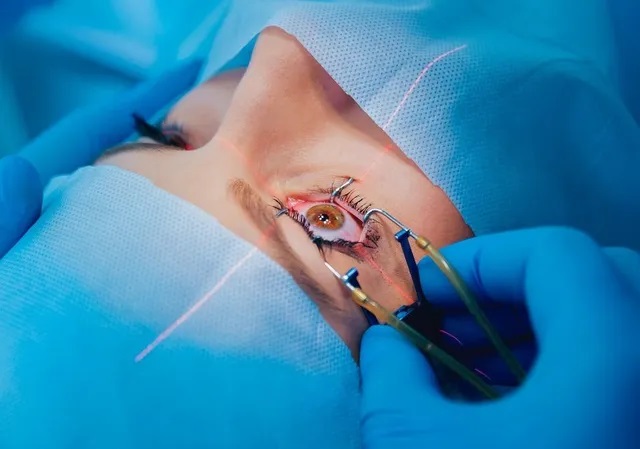
In the operating room, your eye area will be thoroughly cleaned, and sterile drapes will be placed around your head, exposing only the eye. A local anesthetic injection is usually administered, though general anesthesia may be used. An oxygen tube will be placed near your nose to ensure comfort.
Glaucoma
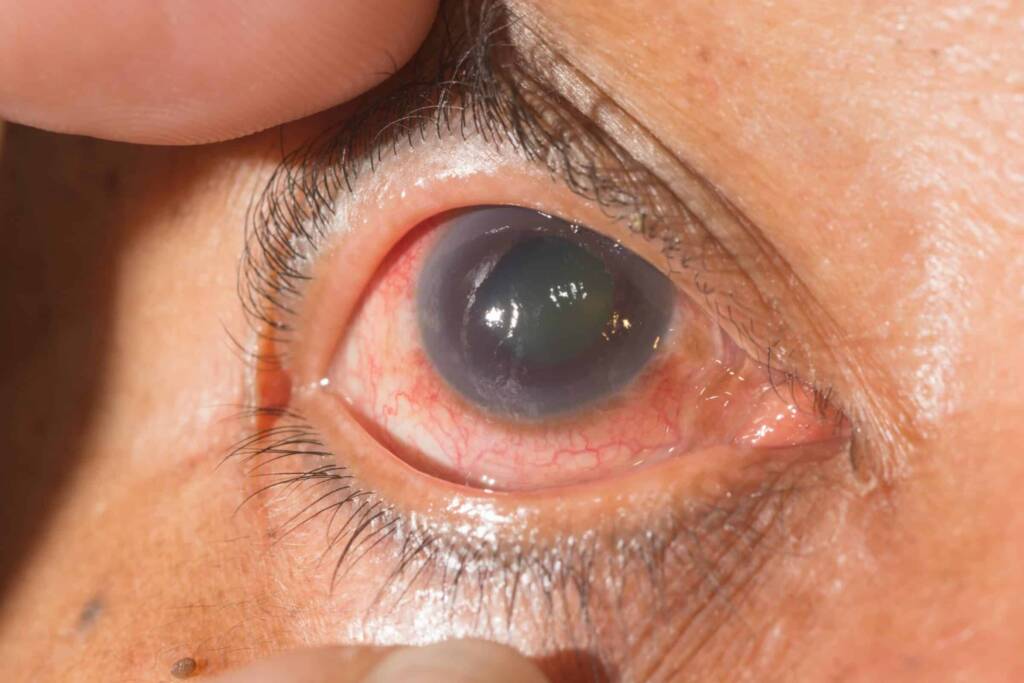
Glaucoma, a disease of the optic nerve, affects around 60 million people worldwide and is the second leading cause of blindness, impacting 7.5 million people. In India, 11 million people are affected, with 1.5 million blind. While there is no cure, doctors can help preserve remaining vision and support a full life.
Cataract
What is a Cataract?
A cataract is a cloudiness of the eye’s natural lens, preventing light from passing through and causing dim or blurred vision. Unlike a growth or film over the eye, a cataract affects the lens inside the eye. The lens focuses light onto the retina, which sends visual information to the brain.
Causes of Cataract:
The most common cause is age-related deterioration of the lens’s structure. Other causes include diabetes, kidney disease, glaucoma, smoking, eye injuries, infections, inflammation, and prolonged use of certain medications. Early symptoms can be managed with new glasses, but as the cataract progresses, vision worsens, and activities like driving and reading become difficult. Symptoms may include glare, colored haloes, or double/multiple images.
Cataracts can develop slowly over years or rapidly within months, often affecting both eyes but not simultaneously. There are no medications, eye drops, or dietary changes that can cure or prevent cataracts. The only effective treatment is surgery, where the clouded lens is replaced with an artificial intraocular lens (IOL), restoring vision close to its original clarity, though glasses may still be needed for reading or driving.
Secondary Cataract
Blurred vision after cataract surgery may not be due to a regrowth of cataract, but rather the clouding of the thin capsular bag membrane. Surgeons can use a laser to clear this cloudiness in a simple outpatient procedure, with no need for stitches or surgery. Improvement in vision typically follows soon after laser treatment.
For any concerns or questions, discuss them with your doctor during your examination. If urgent, contact us via phone, email, or fax. In case of emergency outside regular hours, visit the Institute and provide the patient’s ID, name, and doctor’s name in all communications.
Glaucoma
Glaucoma is often referred to as the “sneak thief of sight” because it gradually reduces the field of vision without noticeable symptoms until it’s advanced.
In glaucoma, there’s an increase in Intraocular Pressure (IOP) due to inadequate drainage of aqueous humor, the fluid inside the eye. This damages the optic nerve, leading to vision loss.
Types of glaucoma include open-angle, angle-closure, and developmental glaucoma, each affecting the eye’s drainage differently. Risk factors include age, family history, steroid use, diabetes, eye injuries, and certain eye conditions.
Diagnosis involves a comprehensive eye exam, including vision tests, slit lamp examination, IOP measurement, and optic disc evaluation. Automated field tests are crucial for detecting visual field loss.
Treatment aims to preserve remaining vision since there’s no cure for glaucoma. Options include eye drops, laser treatment, and surgery, depending on the severity and response to medication.
Regular monitoring is vital to assess disease progression and adjust treatment as needed. Early detection and management are key to preserving vision.
Retina
The eye functions much like a camera, with a lens at the front and a retina at the back, converting visual input into signals for the brain. The macula, at the center of the retina, is crucial for fine vision tasks like reading and recognizing faces, while the surrounding area aids in peripheral vision. Diseases affecting the retina, vitreous, and optic nerve can cause severe vision issues, but modern diagnostics and treatments offer effective management.
Retinopathy of Prematurity (ROP) poses a significant risk to premature infants due to underdeveloped retinas. Early detection by a trained ophthalmologist through pupil dilation and retinal examination is vital. Treatment options like laser therapy or cryopexy can halt the progression of ROP and prevent vision loss.
Laser treatment is a precise method used for various retinal conditions, including diabetic retinopathy, retinal vein occlusion, Age-related Macular Degeneration (AMD), Retinal Breaks, retinal detachment, Central Serous Chorioretinopathy (CSCR), and Ocular Tumors. It helps seal leaky blood vessels, reduce swelling, or repair retinal tears, preserving or improving vision.
Fluorescein angiography and indocyanine green angiography are imaging techniques using colored dyes to visualize retinal blood vessels, aiding in diagnosing and planning treatment for conditions like AMD.
Ultrasonography employs sound waves to create images of the eye’s interior, useful when routine examinations are insufficient.
Scleral buckling surgery is a procedure to reattach a detached retina using a silicone patch, often successful in restoring vision with a low risk of complications. Regular eye examinations, especially for those at risk, can detect retinal issues early, potentially preventing detachment.
Pterygium
A pterygium is a growth of conjunctiva extending onto the cornea, often attributed to prolonged UV exposure, especially common in tropical regions. While many pterygia are asymptomatic, some cause inflammation or irritation. Treatment varies based on size and symptoms, including steroid eye drops for inflammation or surgical removal if vision is threatened or discomfort persists. Surgery involves careful excision and may include techniques to prevent regrowth. Postoperatively, steroid eye drops are often prescribed to reduce inflammation and prevent recurrence. For personalized medical advice, consulting a physician is recommended.
