
Structure of Eye

The eye is a complex organ that converts light rays to images by means of nerve impulses that feed into the brain. To understand the eye and the eye disorders, we can have the eye in two parts – the anterior and the posterior.
- The Anterior of the eye consisting of the Sclera (the white of the eye) and the Cornea.
- The Posterior of the eye consisting of the Retina (the back of the eye), the Optic Nerve (sending impulses to the brain translating the image), the Iris (the fluid containing colored part of the eye) and the Macula (the highly sensitive area of the retina responsible for focusing).
How Eye Works?
- When you look at an object, light rays are reflected from the object to the cornea.
- Light rays pass through the cornea, which does most of the focusing
- The pupil in the Iris opens to let in more light when its dark, and closes to let in less when its bright
- The lens fine tunes the focusing Here at the retina, the light rays are converted to electrical impulses that are then transmitted through the optic nerve, to the brain, where the image is translated and perceived in an upright position.
Cataract
Cataract formation is a natural part of the eye’s aging process.Cataract surgery is a common procedure; most people regain the vision they had earlier with the help of microsurgery. The procedure has a 98% success rate. There is very little discomfort or inconvenience and patients can usually return home few hours after surgery. Here is some general information about what you can expect before, during and after your cataract surgery.
The Surgery
In the operating room, the area around your eye will be cleaned thoroughly.
Sterile drapes will be placed around your head and face, with only the eye exposed. Usually a local anesthetic in the form of an injection is administered next to the eye. Sometimes doctors may have to perform the surgery under general anesthesia. An oxygen tube will be placed near you nose so that you do not feel suffocated.
Glaucoma

Glaucoma is a disease of the optic nerve that affects approximately 60 million people
globally. It is the second most common cause of blindness, leaving an estimated 7.5 million people blind. In India it affects 11 million people, of which 1.5 million are blind.Though there is no cure for this condition, doctors can help preserve remaining vision and enable patients to live a full life.
Cataract
What is a cataract?
Anything you see is an image that enters your eye in the form of light. Inside your eye is a lens, much like the lens of a camera. The lens focuses the light rays coming through the pupil onto the retina at the back of the eye. The different parts of the retina collect this light and send a message to your brain, enabling you to see.
For perfect vision the lens should be clear so that light can pass through it and reach the retina. When the lens becomes cloudy or opaque, light cannot pass through it and the vision becomes dim or blurred. A cloudy lens is called a cataract. A cataract is not a growth or a film over the eye – it is a cloudiness of the natural lens inside your eye.
Causes of Cataract
The most common cause of cataract is the deterioration of the normal structure within the lens of the eye with age. There may be other causes like diabetes, kidney disease, glaucoma, smoking, eye injuries, infection, and inflammation inside the eye. Prolonged use of certain medications can also lead to cataract formation. In the early stages, you can improve your vision by changing your glasses. But once the cataract progresses, changing glasses will not help. You will notice some deterioration in your ability to see things clearly from a distance. You may have difficulty with glare while driving, or while performing activities like reading that require clear vision. Other symptoms may be colored haloes, or double or multiple images in the eye when the other eye is occluded.
A cataract may develop slowly over several years or rapidly within months. Often the other eye will also be affected, but it may not happen at the same time. There are no medications, eye drops, or dietary restrictions that can cure or prevent cataract formation. If the cataract interferes with your regular activities, the only solution is surgery.
In cataract surgery your natural clouded lens is replaced by an artificial intraocular lens (IOL), which helps incoming light rays to be focused properly. Your new lens should restore vision to nearly what it was earlier, though you may need to wear glasses for reading or driving.
Secondary Cataract
Blurred vision, months or years after cataract surgery, leads to the mistaken assumption that the cataract has grown again. This is not a cataract but the clouding of the thin capsular bag membrane that helps keep the lens implant in place.
To restore clear vision surgeons use a laser to open a visual path through the cloudy membrane. This is a simple procedure and is done on an outpatient basis. No stitches or surgery are needed. Your vision should improve soon after the laser treatment.
If you have any concerns or questions, ask the doctor when you come for an examination. If you feel you cannot wait, call or email us, or send a fax, at our numbers given below.
If there is an emergency at night, during a weekend, or on a holiday, come for emergency care to the Institute. Always mention the patient’s ID number, name and the doctor’s name in all your communications.
Glaucoma
What is Glaucoma?
In glaucoma the field of vision decreases so gradually that often the patient does not realize the problem till it is too late. Since it usually causes blindness without any symptoms, glaucoma has been called the ‘sneak thief of sight’.
What Causes Glaucoma?
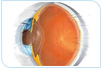
Our eyes constantly produce a clear fluid called aqueous humor (Fig 1 & Fig 2), which bathes and nourishes different regions of the eye (this is different from tears). Normally the fluid drains out of the eye through a ‘drainage canal’ located in the ‘angle’ of the eye (Fig 2), the junction between the cornea and the iris. In persons with glaucoma, the fluid does not drain out as freely as it should, thus increasing the pressure inside the eye, known as intraocular pressure (IOP).
The optic nerve carries all sensations from the retina to the brain. Raised IOP damages the optic disc (that part of the optic nerve that is inside the eye is called the optic disc).
Glaucoma can sometimes occur with a statistically “normal” IOP. Hence the vulnerability of the optic disc is another factor that needs to be considered. Accordingly, the diagnosis of glaucoma requires more than just the mere measurement of intraocular pressure. Types of Glaucoma
There are several types of glaucoma all of which can increase IOP and damage the optic nerve.
In open angle glaucoma, an increase in resistance to the outflow in the canal causes a rise in the IOP. This type develops gradually and the symptoms may not be obvious till the damage has occurred. The patient may lose peripheral vision, leaving only central or ‘tunnel’ vision. This occurs more among people above 45 years of age.
In angle closure glaucoma there is a relative block to the flow of fluid, which causes raised pressure. This occurs more among long-sighted people. In the rarer acute cases, the symptoms are dramatic and may include severe pain in the eye, headache, nausea, reduced vision, and seeing rainbow coloured rings around lights. Stress, anxiety, and reading may also precipitate an attack, which may resolve on its own, but recur after some time.
The more common variety of angle closure glaucoma is chronic angle closure. This behaves similar to open angle glaucoma but here, the ‘drainage’ canal is closed by the iris. The third type is developmental glaucoma, which may be further divided into congenital glaucoma (occurs in infants from the time of birth) and juvenile glaucoma (occurs in children and young adults).
Glaucoma or high IOP may also be secondary and occur due to other causes such as the use of steroid drops without prescription. Such drops should never be used without monitoring the intraocular pressure.
Who is at Risk?
A complete eye examination – not only the usual reading of the chart – is mandatory, especially after the age of 40. Those at risk of developing glaucoma include:
Those above 35 years (the risk increases with age);
People with a family history of glaucoma;
Those who use steroid drops, tablets or ointments;
People with diabetes mellitus, hypertension or who have had eye injuries;
Those who wear ‘minus’ glasses for short-sightedness;
Anyone with complaints of pain, redness, and watering in the eyes; and
People who see colored rings around lights.
Actually, everyone should have a comprehensive eye examination periodically as it can help detect other preventable, controllable, or treatable diseases such as retinal detachment, diabetic eye disease, and cataract.
How is Glaucoma Diagnosed?
Since the treatment methods for open angle and angle closure glaucoma are different, it is important to identify the mechanism involved. The diagnosis (or exclusion) of glaucoma requires a detailed and comprehensive eye examination. Your doctor will do the following examinations:
To detect glaucoma your doctor will conduct the following examinations:
A routine vision test that requires reading letters from a chart,
Slit lamp (microscope) examination: This special microscope is the ophthalmologist’s stethoscope and all patients, not just those suspected of having glaucoma, must undergo a slit lamp examination.
The pressure inside the eye is measured with an ‘applanation tonometer’ attached to the slit lamp. A hand held version of the instrument is also effective. It may be necessary to obtain multiple readings of the pressure during the course of the day and at night. The older method of resting an instrument on the cornea while the patient lies down is not accurate. The newer non-contact air soft (computerized) instrument may be good for screening but cannot be used for diagnosis or for the treatment of glaucoma.
An examination of the angle of the eye is done with the help of a gonioscope. This is a contact lens placed on the eye to examine the angle of the eye. Its use is mandatory in determining the type of glaucoma – open angle or angle closure.
The above two steps require the use of drops to eliminate sensation in the eye. The drops may burn a little bit.
An optic disc examination on a dilated eye is also required. The doctor will usually administer eye drops to dilate the pupil, facilitating an examination of the optic disc and the back of the eye, the retina. For obtaining a stereoscopic view on the microscope, a hand-held lens or a contact lens is the best method. A computerized scan of the optic disc may also be done.
To confirm the diagnosis, the doctor will conduct an automated field or perimetry test. Damage to the optic nerve limits the field of vision, but regular vision, i.e. the ability to read an ophthalmologist’s eye chart, is affected at a much later stage. In its early stages glaucoma can only be detected or monitored by using an automated perimetry test. A normal patient will have a ‘full field vision’, while a person with glaucoma has black, non-seeing areas in the field of vision.
Many people have difficulty doing the perimetry test at first, and may be better at it the second or the third time. Baseline tests are necessary for future comparison and periodic examinations are essential to check the progression of the disease.
Considering the importance of the test, ANY automated perimeter is NOT acceptable. The field test is a subjective test and it is important to have a calibrated machine with an appropriate normal database against which to compare your results.
Sometimes a diagnosis may not be possible on one visit. In very early cases it may be necessary to repeat the entire examination after a period of observation.
Treatment
It is important to realize that there is no cure for glaucoma. Once nerve fibers die and visual function is lost, it cannot be recovered. Treatment can only help preserve remaining vision; hence it is imperative to detect the disease in its earliest stage.
The management of glaucoma must be an individualized effort. Simplistically speaking, in angle closure glaucoma doctors use a laser to create an alternative path for the fluid to drain out. However, this approach works for early cases; advanced cases require medication and surgery as for open angle glaucoma. An attack of closed angle glaucoma is an emergency and the IOP must be lowered as soon as possible to prevent damage to the optic nerve.
For open angle glaucoma, initially eye drops are used to lower IOP; your doctor will select the one most suited for your condition. If the disease is advanced, and/or medical treatment fails, surgery may be necessary.
Medical therapy is expensive, and likely to be life-long. As with any treatment, there is a risk of side effects. Sometimes the side effects may be more uncomfortable for the patient, and less acceptable, than living with the disease. Therefore doctors consider the risk-benefit ratio of the treatment options for glaucoma. The main criterion is how much functional capacity is affected rather than the actual degree of vision loss. Your doctor will select the treatment most suited for your condition, please follow the advice meticulously.
In some patients glaucoma may be controlled by medicine alone, while others may need laser treatment or surgery. Surgery usually involves cutting a piece of tissue from the angle of the eye and allowing the fluid to accumulate under the transparent skin that surrounds the eyeball. However, glaucoma surgery is not as predictable as cataract surgery and carries more risks, including loss of the eye from devastating bleeding or infection. It is usually used if drugs fail to control eye pressure, or for socioeconomic considerations.
Non-penetrating surgery can also help decrease eye pressure and has fewer complications than the standard approach. But its results are not as good. Hence it is not a first line of treatment for glaucoma.
In cases with poor potential for visual recovery or function, a different kind of laser may be used to reduce eye pressure. This is usually reserved for advanced cases.
Need for Constant Care
Life long monitoring is essential, the frequency of follow up visits depends on the individual case. At each visit most of the tests may be repeated to determine the progression of the disease and to decide whether change in treatment is needed.
Retina
The eye is like a camera with a lens in front and a film (retina) at the back. The retina is located approximately two centimeters behind your pupil. It is shaped like a small cup. The retina converts the ocular image into a signal that is sent to the brain. The central part of the retina, called the macula, is used for straight-ahead vision and what is in your direct line of sight.
A healthy macula is crucial for tasks involving fine vision such as reading, recognizing faces and distinguishing things. The area surrounding the macula helps in mobility and in seeing from the ‘corner’ of the eye, though it is not useful for fine work. The retina is connected to the brain by the optic nerve. Blood is supplied to the retina and the optic nerve by blood vessels that maintain the health of these tissues. In front of the retina is the vitreous cavity, which is filled with a gel-like substance, called the vitreous.
Diseases of the retina, the vitreous, and the optic nerve can cause serious vision problems. Fortunately, most of them can now be managed satisfactorily with modern methods of diagnosis and treatment.
This link will help you understand the treatment of diseases of the retina and the vitreous. Remember, early diagnosis and prompt and appropriate treatment can result in a better outcome.
Retinopathy of Prematurity
Why should I worry about the eyes of a premature baby?
The inside of the eye, the retina is not fully developed in premature babies. Abnormal blood vessels can develop in such a retina. These abnormal blood vessels can cause internal bleeding and even retinal detachment. This is called Retinopathy of Prematurity (ROP). This condition results in low vision or blindness – both of which are irreversible.
How can we detect ROP?
A trained ophthalmologist can detect ROP by dilating the pupils of the eye using eye drops. An indirect ophthalmoscope is used to scan the entire retina to detect ROP and gauge the state of retinal maturity.
Do all babies need a retinal examination for ROP?
Babies with a birth weight of less than 1700 grams or those born in under 35 weeks of pregnancy are most likely to have ROP. Pre-term babies who have had problems after birth such as lack of Oxygen, infections, blood transfusions breathing trouble, etc., are also vulnerable.
Is it too late for my baby’s eyes?
Follow the “Day-30” strategy. The retinal examination should be completed before “day-30” of the life of a premature baby. It should preferably be done earlier (at 2-3 weeks of birth) in very low weight babies (1200 grams birth weight).
What is the treatment for ROP?
ROP is treated with Laser rays or a freezing treatment (Cryopexy). The treatment helps stop further growth of abnormal vessels thus preventing vision loss.
How often should the retina be examined?
ROP can progress in 7-14 days and therefore, needs a close follow-up till the retina matures.
When should we treat ROP?
ROP needs to be treated as soon as it reaches a critical stage called Threshold ROP. There is 50% or greater risk of vision loss if left untreated after this. Time is crucial!
After treatment
If treated in time, the child is expected to have reasonably good vision. All premature babies need regular eye examinations till they start going to school.
They may need glasses or treatment for lazy eyes/ cross-eyes and sometimes, for cataract, glaucoma and retinal detachment.
Laser Treatment of the Retina
A laser is a pure, high-intensity beam of light energy. The laser light can be precisely focused onto the retina, selectively treating the desired area while leaving the surrounding tissues untouched. The absorbed energy creates a microscopic spot to destroy lesions or weld tissues together.
Laser surgery is usually painless; at the most it may cause temporary discomfort. It is usually performed in the operating room while the patient is awake and comfortable. In rare cases, anesthesia is given those patients who cannot tolerate the discomfort or to children to keep them still during treatment. The entire procedure lasts 10 to 30 minutes.
Who requires laser treatment?
Lasers are commonly used to treat the following eye conditions:
Diabetic Retinopathy
The retinal blood vessels are like pipes, bringing blood into and taking it out of the back of the eye. In diabetes, however, the vessels may leak, causing the retina to swell and not work properly. When the swelling involves the central area of retina vision may be affected. (This is known as diabetic macular edema.)
Laser treatment can seal the leaks, thereby preventing further vision loss. In some patients new retinal blood vessels may grow, which will replace some of those that have closed due to diabetes. (This is known as proliferative diabetic retinopathy). This new retinal blood vessel, unlike the normal blood vessel, has a tendency to bleed inside the eye, resulting in decreased vision. Laser treatment can often prevent severe vision loss by making these new vessels regress.
Retinal Vein Occlusion
The small blood vessels that drain the blood from the retina (retinal veins) can sometimes get blocked (retinal vein occlusion). This is more common in patients with diabetes or high blood pressure. A retinal vein occlusion can cause the retina to swell with fluid and blood, blurring central and peripheral vision. At other times, new blood vessels may grow and cause pain as well as very high pressure inside the eye (neovascular glaucoma).
Laser treatment can help reduce this swelling or cause the new blood vessels to disappear.
Age Related Macular Degeneration (AMD)
With age, some people may develop changes in the macula, the portion of the retina responsible for our central reading vision. Most people develop the dry type of AMD, which usually causes gradual vision loss. The more severe or wet type causes the macula to swell with fluid and blood. Symptoms of wet macular degeneration include painless, blurred and distorted vision. Urgent laser surgery can sometimes prevent or delay vision loss in patients with wet AMD. While the off central wet AMD patients benefit from thermal laser treatment, those with central vision problems need a prior injection of Visudyne. This is known as photodynamic therapy.
Retinal Breaks and Retinal Detachment
The retina lines the back of the eye like a wallpaper. Retinal tears or rips can occur as part of an aging phenomenon, or following an intraocular surgery or eye injury. When a retinal tear develops, patients often see cobweb-like floaters or light flashes. The liquid that normally fills the central portion of the eye (the vitreous) can leak beneath the tear, lifting the retina away from the eye wall. This is called a retinal detachment, which if left untreated can cause blindness. Often laser surgery around retinal tears before the fluid accumulates enables surgeons to weld the retina to the underlying eye wall. This can prevent or limit retinal detachment.
Central Serous Chorioretinopathy (CSCR)
Central Serous Chorioretinopathy consists of one or more ‘blisters’ of fluid (serous detachment) beneath the macula. It can cause reduction and distortion of vision, abnormal color vision, central scotoma, and temporary hyperopia or far-sightedness. Although the vast majority of cases resolve on their own, laser photocoagulation is sometimes necessary for persistent lesions and in those patients who require early visual rehabilitation.
Ocular Tumors
Some patients may have non-cancerous leaking vascular tumors that can cause the retina to swell and not function properly. Laser surgery can destroy some of these tumors and make the swelling go away.
How do I know that I require laser treatment?
With retinal diseases your eye will almost always look and feel normal, even when there is bleeding and leakage in the back of the eye. Your vision may also be normal for a while despite the presence of potentially blinding eye problems.
The only way to find out whether you need laser surgery is to have careful, dilated retinal examinations at regular intervals, often followed by a special test (called fluorescein angiography if advised by the retinal specialist), to evaluate the eye’s circulation.
After laser surgery
There are virtually no restrictions following retinal laser surgery, but you would need to relax on the day of the treatment. Most patients find they can go back to their routine a day later. Invariably the doctor will advise you not to lift heavy weights for a few weeks. In some cases the doctor may advise patients to stay at home for several days. You will be required to come again for a follow-up examination in a couple of weeks up to a couple of months.
Most patients notice no changes in vision following their laser surgery, although there may be some temporary blurring for several weeks or even months. In addition, depending on the condition being treated, some patients may notice a permanent blind spot or decrease in peripheral and night vision.
Is one session of laser treatment enough?
The number of sessions required by a patient depends on the disease for which the laser treatment is done. It takes usually several weeks to months for surgeons to decide whether the treatment has been successful. Many patients require more than one session of treatment to control their problem and prevent further loss of vision. Freezing or Cryo Treatment of the Retina
What is cryosurgery?
‘Cryo’ means extremely cold or freezing. This operation employs a delicate instrument that freezes small spots which are transformed into pinpoint scars that strengthen the retina. The temperature required for cryosurgery is approximately minus 70 degrees centigrade.
What are the do’s and don’ts after cryosurgery?
Generally patients can return to their normal routine the following day. But they are advised to relax on the day of surgery. In cases where there has been a tearing of the retina, the surgeon may ask patients to limit their activities for at least ten days. The restrictions may include the following:
- If an eye pad was used after the cryosurgery, it should be removed after one day of use.
- Do not bend over so that your head is below your waist.
- Do not lift anything that weighs more than five kilograms.
- Avoid rubbing the affected eye.
- Avoid strenuous activities: you may cook or wash dishes, but no housework that involves bending or lifting weights.
- You may watch television or read.
- Alcoholic beverages should be avoided.
- No sexual intercourse.
- No automobile trips except to the doctor’s office.
What are the effects of cryosurgery?
Temporary side effects include blurred vision, redness of the eye, mild pain, watering, double vision, swelling of eyelids or a dilated pupil. These side effects usually clear up within a few weeks. Most patients respond favourably to this operation, but a small percent of patients may not.
What are the possible complications?
All surgery has some possible complications but fortunately, the occurrence of such problems with cryosurgery is infrequent. At least 99% patients have no complications. The complications that may occur include bleeding within the eye or retinal detachment. There is the very rare possibility that all vision might be lost. Diabetic Disease of the Retina
How does diabetes affect the retina?
Most persons suffering from diabetes develop changes in the retina over a period of time. This is caused by damage to the small blood vessels (or capillaries) in the retina.
What can I do to limit the diabetic damage to my retina?
You should consult the doctor treating you for diabetes regularly and follow all instructions regarding diet and medication. It is a fact that only strict control of blood sugar will help minimize damage to the retina. Frequent examination of the retina after full dilation of the pupil can help detect retinopathy early, leading to better treatment outcomes. This retinal examination should be done periodically even if your vision is clear.
Can diabetes affect other parts of the eye?
Retinal changes are the major problem, but at times diabetes can also cause a rise in eye pressure (glaucoma), clouding of the lens (cataract), and weakness of the optic nerve or eye muscle. Cataracts often occur at a younger age in diabetic patients. Glaucoma can cause damage to the optic nerve. In fact diabetes is one of the several possible causes of glaucoma.
Damage to the small vessels of the optic nerve can affect vision, and weakness of the eye muscles may cause double vision. A diabetic is also more likely to develop sudden vision loss due to occlusion of the retinal vessels (branch or central retinal vein occlusion), bleeding in the vitreous cavity, detachment of the retina, or infections of the cornea and vitreous.
How does diabetic retinal disease (diabetic retinopathy) affect the vision?
Swelling (edema) in the central part of the retina (macular edema) can cause blurring of fine vision. Fragile new blood vessel sprouts may break and bleed into the interior of the eyeball, causing blurring of the entire field of vision. In the early stages of the disease the vision remains good therefore, the disease may escape notice. That is why it is essential to have regular retinal examinations if you know that you have diabetes.
How can this disease be treated?
Swelling of the central part of the retina may be controlled with limited laser treatments. Sometimes one laser session will suffice, though some patients require several sessions. Abnormal blood vessel sprouts require extensive laser treatment involving 2,000 to 3,000 laser spots, i.e., three or more laser sessions. More acute problems with severe bleeding or retinal detachment require surgery such as scleral buckling or vitrectomy or both.
What are the results of the treatment?
Limited laser treatment in the central zone of the retina is designed to reduce the amount of future visual loss, but the lost vision cannot be restored. Extensive laser treatment for fragile blood vessel sprouts usually prevents a large bleed within the eye, thereby preventing major loss of vision. Vision loss from severe bleeding in the eye or retinal detachment can usually be improved with surgery, but some patients may not respond to the treatment. Because we have as yet no cure for diabetes, it may continue to damage the retina even after laser treatment or even if the blood sugar level is controlled. Patients with diabetic retinopathy need life-long regular follow-ups after treatment.
What are the complications of the treatment?
Most patients do not have any complications but occasionally, laser treatment may cause temporary pain or blurred vision since the effect of the treatment is seen only 4-6 weeks later. Mild or severe haemorrhage or retinal detachment can also occur. Such complications are occasionally seen after major eye operations and may very rarely lead to loss of complete vision.
Photography of the Retina with Dye
Fluorescein Angiography and Indocyanin Green Angiography
What is fundus angiography?
Fluorescein and indocyanine green angiography are tests that use special cameras to photograph the structures in the back of the eye. These tests are very useful for locating the damage to the blood vessels that nourish the retina (light sensitive tissue) and in turn, checking on the health of the retina itself. In both tests, a colored dye is injected into a vein in the arm of the patient. The dye travels through the circulatory system and reaches the vessels in the retina and those of a deeper tissue layer called the choroids. Neither of the tests uses any harmful forms of radiation.
Fluorescein is a yellow dye, which glows in visible light. Indocyanine is a green dye that fluoresces with invisible infrared light; it requires a special digital camera sensitive to these light rays This indocyanine green angiography helps your doctor make the correct diagnosis and plan the best course of treatment especially in diseases like age related macular degeneration (AMD).
How is fundus angiography done?
Before the procedure, you will be asked questions about your general health and the medications that you are using. A self-explanatory consent form, which explains the side effects in detail, will be provided to you. You will have to give your consent before the procedure. You should have a light meal before undergoing the procedure and must be accompanied by a family member or friend.
Eye drops will be administered to enlarge the pupils — this takes approximately 30 minutes. You will then be asked to sit still in front of the camera while a series of color photographs of your eyes are taken. You will be given an injection in your arm, and more photographs will be taken.
The test takes approximately 15-30 minutes.
What are the side effects?
Both fluorescein angiography and indocyanine green angiography are considered very safe and serious side effects from these tests are uncommon. However, there is the possibility that a patient may have a reaction to the dyes. While fluorescein contains no iodine and is safe in patients known to be allergic, indocyanine green is currently formulated with iodine and should not be used in individuals with any known allergies. Some people may experience slight nausea after the dye injection, but the feeling usually passes quickly. Patients who are allergic to the dye can develop itching and a skin rash. These symptoms generally respond quickly to oral medications such as anti-histamines or steroids. Very rarely, a sudden life-threatening allergic reaction called anaphylaxis can occur. This condition requires medical treatment.
There is also the possibility of an infiltrate of the dye into the skin at the injection site; this may cause some discomfort or discoloring of the skin for several days. The fluorescein dye will turn the patient’s urine orange and may slightly discolor the skin as well for a brief period. Your physician can explain the individual risks of these procedures for certain patients, including pregnant women.
Sound Wave Echo Pictures of the Retina with Ultrasonography
What is ultrasonography?
This is a painless test that makes use of sound waves which bounce back or echo from the interior of the eye to create a clear picture of the anatomy of the eye. This test is needed when details of the eye cannot be seen with the instruments used in routine examinations. How is the test performed?
You will be given eye drops to prevent pain and thick jelly will be placed on the eye. The ultrasound instrument is then gently placed on the eye. The test takes about 10 minutes and results in a picture of both the normal and abnormal anatomy of the eyeball. It is a safe and painless procedure, no X-ray exposure occurs in this test.
How is the ultrasound test used?
Your doctor can use these echo pictures to arrive at a diagnosis, the probable future health of your eye, and a treatment plan. However, the test will only reveal the structure of the eye.
What complications are likely to occur?
There are no significant complications, but there may be some temporary pain of the eyeball if it is inflamed. This can be easily treated by your doctor with no permanent side effects.
Repair of Retinal Detachment with Scleral Buckling
What is retinal detachment?
Normally the retina is firmly attached to the back of the eyeball. If it becomes detached, the eye loses vision. This is a rare disease occurring in about one person out of 10,000, each year. The immediate cause is usually a hole in the retina. It may be due to injury or surgery, but is usually due to weakness of the retina. This is sometimes called degeneration.
What is scleral buckling surgery?
The surgery may be done under general anaesthesia (you will be sound asleep) or local anaesthesia (you will be awake but an injection will prevent any pain). The retina is reattached by freezing (cryosurgery) and with the placement of a permanent silicon patch (buckle) on the wall of your eyeball. The external stitches will melt away and do not have to be removed. Usually the eye responds to one operation; occasionally, additional surgery may be required. The eyelashes are cut before surgery but they always grow back. You will probably spend one or two nights in the hospital after the operation. Normally, only the operated eye is bandaged but, sometimes, both eyes may be bandaged for a few days. Most patients can return to work in four to five weeks.
What may I do after surgery?
You must stay at home for at least three weeks, traveling should be avoided except to visit the doctor. After surgery you will be given written instructions regarding medication and precautions to be taken. You should carefully observe these instructions. You may be advised to lie on your side or stomach while sleeping or resting.
What are the chances of success?
In most cases (85%) the retina can be reattached with a single operation. Occasionally additional surgery is necessary; this brings the final cure rate up to approximately 95%. The final degree of clarity of vision will not be known for three months. If you had lost your reading vision before surgery, you should find considerable improvement but probably not 100%. If your reading vision was not lost before surgery, good vision will be retained (after convalescence) in more than 90% cases. In 5% cases the retina may not re-attach, necessitating further surgery.
What are the common side effects and complications of the surgery?
Your vision will be blurred. The eye will be painful, red and swollen and there may be some mucus discharge. The pupil will be large and you may see double. These side effects are usually temporary and last only a few weeks. In many cases the eye will become more near-sighted; this can be corrected with spectacles.
Over 90% cases have no significant complications. Occasional problems include bleeding or infection or re-detachment. Very rarely such complications could lead to the loss of all vision. Anaesthesia-related complications are also rare; the anesthetist will discuss these with you.
What about the future of my retina?
If the retina remains attached for three months after surgery, the chance of recurrence is only 10%. If the retina of your other eye appears normal at this time, the chance of developing a detachment later on is approximately 12% in the eye that has not been operated.
Can retinal detachment be prevented?
In some cases the retina is more fragile and prone to formation of holes or breaks. If these are detected and sealed in the early stages by laser or cryosurgery, retinal detachment can be prevented. People who are likely to develop retinal detachment should have periodic examinations done after dilation of the pupils. Some of the situations where this is desirable are:
- History of detachment in one eye
- Family history of retinal detachment
- History of injury to the eye or its surrounding bones
- History of flashes and floaters
- Sudden onset of floaters or change in the character of floaters
Pterygium
What is a pterygium?
A pterygium is a wedge-shaped fibrovascular growth of conjunctiva (the surface tissue of the white of the eye) that extends onto the cornea. Pterygia are benign lesions that can be found on either side of the cornea.
What causes a pterygium to form?
It is thought that prolonged exposure to ultraviolet light may contribute to the formation of pterygia. Pterygia are more often seen in people FROM tropical climates, but can be found in others as well.
What symptoms would I have FROM a pterygium?
Pterygia are often asymptomatic, and many do not require immediate treatment. However, some pterygia become red and inflammed FROM time to time. Large or thick pterygia may bother some people due to a persistent foreign body sensation in the eye.
What is the treatment for a pterygium?
This depends largely on the size and extent of the pterygium, as well as its tendency for recurrent inflammation. Evaluation by an ophthalmologist will help determine the most optimal treatment in each case. If a pterygium is small but becomes intermittently inflammed, your ophthalmologist may recommend a trial of a mild steroid eye DROP during acute inflammatory flares. If these drops are recommended, you should remain under the care of your ophthalmologist to ensure that you do not develop side effects FROM the use of these medications. In some cases, your ophthalmologist may recommend surgical removal of the tissue.
When should a pterygium be surgically removed?
This will depend largely on the judgment of your physician. Removal will likely be advised if the pterygium is growing far enough onto the cornea to threaten your line of vision. Pterygia may also be removed if they cause a persistent foreign body sensation in the eye, or if they are constantly inflammed and irritating. In addition, some pterygia grow onto the cornea in such a way that they can pull on the surface of the cornea and change the refractive properties of the eye, causing astigmatism. Removing the pterygium may decrease the astigmatism.
What is involved in the surgical removal of a pterygium?
The removal may take place in a procedure room or operating room setting. The pterygium is carefully dissected away. In ORDER to prevent regrowth of the pterygium, your ophthalmologist may remove some of the surface tissue of the same eye (conjunctiva) and suture it INTO the bed of the excised pterygium. Alternatively, an antimetabolite such as mitomycin may be applied to the site. Postoperatively, your ophthalmologist may recommend some steroid eye drops for several weeks to decrease the inflammation and prevent regrowth of the pterygium.
The information and recommendations appearing on these pages are informational only and is not intended to be a basis for diagnosis, treatment or any other clinical application. For specific information concerning your personal medical condition, the DJO suggests that you consult your physician.

